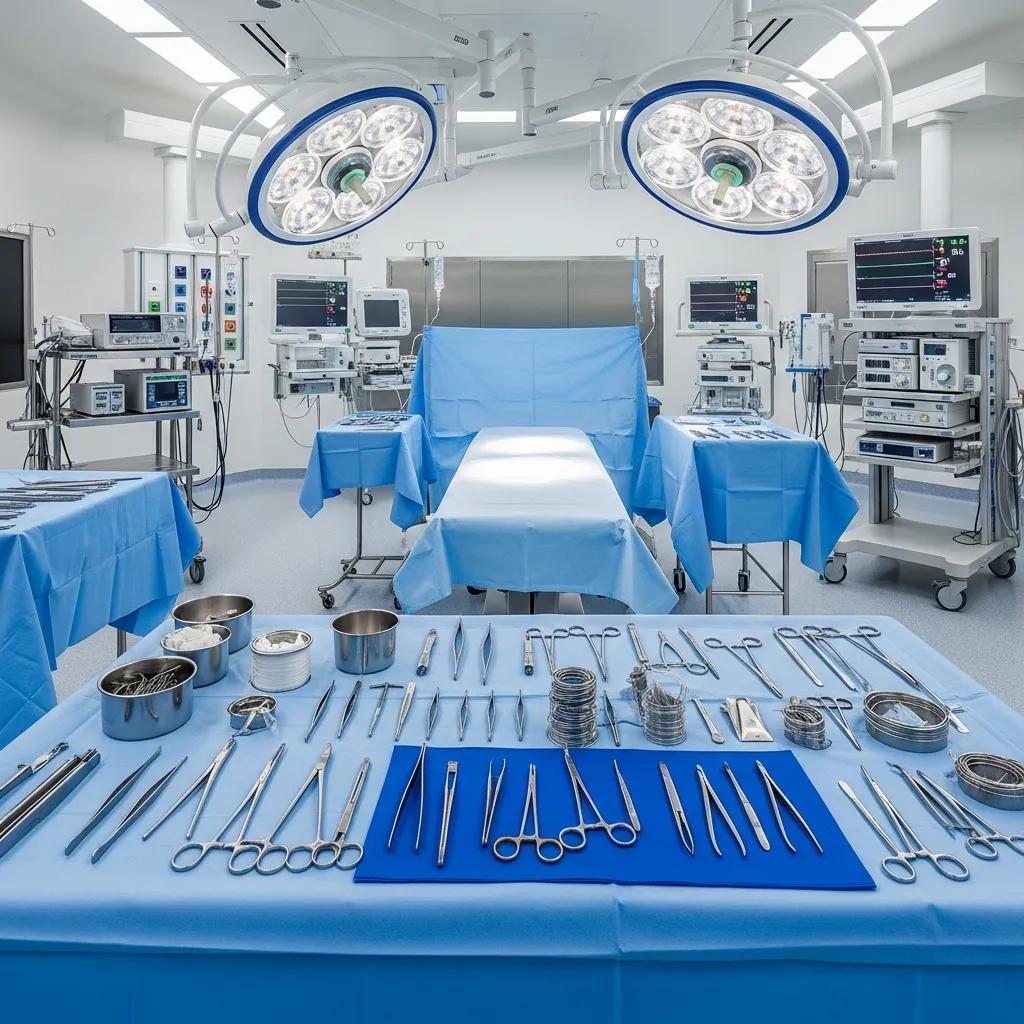
Surgical Suite Cleaning and Sterilisation Procedures for Infection Control
Surgical suite cleaning and sterilisation encompass systematic processes that reduce bioburden, remove contaminants, and maintain a sterile environment to prevent healthcare-associated infections (HAIs). This guide explains core procedures—from pre-operative preparation and between-case turnover cleaning to terminal cleaning and instrument handover—while connecting procedures to regulatory expectations and practical monitoring. Readers will learn step-by-step workflows, the disinfectants commonly used in operating theatres, verification methods such as ATP testing, and how staff training and PPE use reduce contamination risk. The article also outlines relevant international and Australian guidance that informs protocols and describes how a local provider customises plans for medical facilities. Practical lists, comparison tables of disinfectants and area-specific cleaning recommendations, and quality assurance measures are included to help clinical managers, infection prevention teams, and facility operators implement robust sterile environment maintenance.
What Are the Essential Steps in Surgical Suite Cleaning?
Surgical suite cleaning is a staged workflow designed to control contamination through defined phases: pre-operative preparation, between-case turnover cleaning, post-operative cleaning, and terminal cleaning after the last case. The mechanism relies on source control (removal of gross soil), targeted disinfection of high-touch surfaces, and validated dwell times to inactivate pathogens, resulting in reduced infection transmission and readiness for subsequent procedures. Implementing top-to-bottom and clean-to-dirty sequencing preserves sterile zones and prevents recontamination of critical equipment, and staff allocation differs between rapid turnover and full terminal cycles. Time estimates and staffing models are critical for efficient perioperative operations; understanding when to escalate from turnover to terminal cleaning prevents compromise of aseptic conditions and supports scheduling reliability.
Surgical suite cleaning typically follows these numbered operational steps:
- Prepare and don appropriate PPE; remove disposable waste and gross contamination to reduce bioburden rapidly.
- Perform targeted turnover cleaning on high-touch surfaces and visible equipment between cases to restore procedural readiness.
- Conduct post-operative cleaning tasks that include floor care, bed and cart decontamination, and safe instrument handover to reprocessing.
- Execute terminal cleaning after the last case or contamination events, covering floor-to-ceiling surfaces, vents, and ancillary spaces with validated disinfectants.
This structured approach clarifies responsibilities and aligns cleaning intensity with patient risk, while the next sections explain terminal cleaning techniques and the differences between turnover and terminal cycles.
How Does Terminal Cleaning Ensure Operating Room Sterility?

Terminal cleaning is a comprehensive deep-clean performed after the final scheduled procedure or when contamination is suspected, aiming to remove settled dust, disinfect all surfaces, and reduce residual microbial load to meet sterility thresholds. The process typically begins with a full visual inspection and removal of gross soil, followed by methodical cleaning of overhead fixtures, surgical lights, horizontal surfaces, equipment casings, ventilation grills, and floors using TGA-approved or equivalent disinfectants applied with manufacturer-recommended dwell times. Verification methods such as ATP luminometry, periodic microbial swabs, and documented checklists provide objective evidence of cleanliness and identify recurrent problem areas for corrective action. Common pitfalls include inadequate dwell time, cross-contamination from cleaning tools, and omission of vertical surfaces; strict SOPs and supervised QA checks mitigate these risks and preserve operating room sanitation.
Terminal cleaning protocols must be validated and documented to ensure repeatability and traceability, linking each procedural step to verification evidence and corrective actions when metrics fall outside acceptance criteria. The following subsection details rapid between-case cleaning and how to determine when escalation to terminal cleaning is required.
What Is Turnover Cleaning and When Is It Performed?
Turnover cleaning is a focused, time-sensitive process performed between surgical cases to restore the immediate clinical zone—operating table, mayo stand, monitors, and high-touch points—to a condition safe for the next patient. The mechanism targets visible soil and frequently touched surfaces with rapid-acting disinfectants, using a wipe-discard-wipe method to avoid cross-contamination; typical turnover durations range from 10 to 30 minutes depending on case complexity and staffing. A concise checklist for turnover cleaning improves speed and consistency: disinfect bed rails and controls, wipe monitors and touchscreens, replace drapes if needed, and ensure instrument trays are intact or exchanged with sterile sets. Escalation to terminal cleaning is indicated after exposure to significant contamination, an uncontained bodily fluid spill, or when an airborne or contact-transmissible infection is suspected.
Efficient turnover cleaning balances speed with thoroughness by prioritising high-risk surfaces while reserving deep-clean cycles for terminal procedures; this distinction supports predictable theatre throughput and protects aseptic integrity during successive operations.
Which Hospital-Grade Disinfectants Are Used in Surgical Theatre Disinfection?

Choosing hospital-grade disinfectants for the operating theatre requires matching product class, active ingredient, and validated dwell time to the target organisms and surface compatibility; common classes include quaternary ammonium compounds (QACs), hydrogen peroxide formulations, alcohols, and chlorine-based agents. Selection criteria emphasise broad-spectrum efficacy, compatibility with medical devices and surfaces, label-approved contact times, and regulatory approvals relevant in Australia such as TGA considerations for disinfectant claims. Application methods vary by agent and risk level: wipe-discard-wait for contact surfaces, spray-then-wipe for complex shapes, and non-contact methods (e.g., aerosolised hydrogen peroxide or UV-C) as adjuncts where validated. Practical comparisons help infection prevention teams weigh pros and cons.
The table summarises disinfectant classes used in surgical theatre cleaning and their practical attributes for selecting an appropriate agent.
| Disinfectant Class | Active Ingredient | Typical Contact/Dwell Time | Notes |
|---|---|---|---|
| Quaternary ammonium compounds (QACs) | QAC blends | 1–10 minutes depending on formulation | Good surface compatibility; limited sporicidal activity |
| Hydrogen peroxide formulations | H2O2 (stabilised) | 1–10 minutes; accelerated forms shorter | Broad efficacy including some spores when higher concentrations used |
| Alcohols (70% isopropyl or ethanol) | Isopropyl alcohol, ethanol | 30 seconds–2 minutes | Rapid bactericidal/virucidal action; not residual and not suitable for large area surfaces |
| Chlorine-based (sodium hypochlorite) | Sodium hypochlorite | 1–10 minutes depending on concentration | Broad spectrum including spores at higher strengths; corrosive to some surfaces |
What Are the Efficacy and Dwell Times of TGA-Approved Disinfectants?
Efficacy and dwell time depend on the active chemistry and label claims, with TGA considerations in Australia emphasising that disinfection claims must be supported by validated testing and instructions for use. For example, alcohols act quickly but provide minimal residual action and are unsuitable for porous surfaces, whereas hydrogen peroxide and higher-strength chlorine agents offer broader pathogen coverage with longer dwell requirements for some organisms. Operational scheduling must account for verified contact times to avoid false security; using a shorter-acting product without waiting the required dwell time will reduce efficacy and can increase HAI risk. Surface compatibility assessments and spot testing prevent damage to delicate equipment while ensuring infection prevention.
Adherence to label instructions and documentation of dwell time compliance are QA priorities, as they directly affect microbial reduction and inform audit results that guide continuous improvement.
How Do Eco-Friendly Disinfectants Balance Safety and Sustainability?
Eco-friendly disinfectants aim to reduce environmental toxicity while maintaining sufficient antimicrobial performance for given applications, often utilising hydrogen peroxide, enzymatic cleaners, or plant-derived surfactants with lower persistence in the environment. The trade-off can be reduced spectrum or longer dwell times compared to conventional chemistries, so their use should be targeted to low-risk areas or combined with validated protocols for higher-risk surfaces. Sustainable procurement and selection involve comparing efficacy data, lifecycle assessments, and facility priorities—select eco-options where microbiological data support use, and retain hospital-grade agents for critical surfaces in the surgical field. Providers that prioritise environmental consciousness integrate greener chemistries where appropriate and maintain a safety-first approach for perioperative infection control.
When eco-friendly agents are considered, policy should define where they are acceptable and where conventional hospital-grade agents remain mandatory to preserve sterile environment maintenance.
How Does Divine Commercial Cleaning Customise Surgical Suite Sterilisation Procedures?
Divine Commercial Cleaning provides tailored sterilisation procedures for medical facilities by combining risk assessment, standard operating procedures, and ongoing quality assurance to meet perioperative hygiene needs. The company focuses on customised solutions delivered by experienced professional cleaners who undergo relevant training and police checks, offering flexible engagement without lock-in contracts and backed by a money-back guarantee. Service delivery emphasises local expertise from Maroochydore, QLD and operational coverage across the Sunshine Coast and Brisbane, allowing rapid responsiveness to facility schedules and infection prevention priorities. Documentation, verification, and continuous improvement are integral to their approach, aligning cleaning intensity with clinical risk and regulatory expectations.
What Is the Six-Step Cleaning Process Tailored for Medical Facilities?
Divine Commercial Cleaning implements a six-step process designed to deliver consistent sterile environment maintenance for medical settings: assessment, plan development, execution, verification, documentation, and continuous improvement. Assessment begins with a risk analysis of theatre layout and traffic, informing SOP development and scheduling. Plan development produces custom checklists, dwell time charts, and equipment compatibility notes to guide frontline teams. Execution covers trained staff performing cleaning with proper agents and techniques timed to theatre flow. Verification uses ATP and audit checklists; documentation records outcomes and corrective actions. Continuous improvement reviews data to refine SOPs and training cadence.
Each step includes deliverables—risk assessment reports, written SOPs, audit logs, and retraining records—to ensure transparency and measurable performance that integrates with facility infection control governance.
How Are Quality Assurance and Documentation Managed?
Quality assurance integrates objective monitoring tools, routine audits, and record-keeping to confirm that cleaning processes meet specified standards; key metrics include cleaning completion rates, dwell time adherence, ATP results, and checklist sign-offs. Scheduled audits—daily operational spot checks and quarterly comprehensive reviews—allow trending of ATP or microbial swab data and identification of persistent problem areas for targeted retraining. Documentation templates include signed cleaning logs, incident reports, verification photos, and corrective action records that provide traceability and support regulatory inspections. Escalation procedures define thresholds for immediate remedial action and clinical notification in the event of non-conformance or potential exposure incidents.
This structured QA framework ensures accountability and creates a feedback loop for process improvement, linking frontline performance to measurable outcomes and facility safety objectives.
Which Standards and Guidelines Govern Operating Room Cleaning Protocols?
Operating room cleaning protocols are informed primarily by international best-practice guidance such as AORN and CDC documents, and by Australian national and state-level regulatory frameworks that influence disinfectant selection and record-keeping. These sources recommend cleaning frequency, surface-specific methods, PPE usage, and verification strategies that collectively define a compliance baseline for perioperative services. Mapping local SOPs to these references ensures consistent adoption of evidence-based methods while allowing necessary adaptation for facility specifics such as theatre design, ventilation, and patient acuity. Understanding the interplay between international guidance and Australian regulatory requirements is essential for compliance and for demonstrating due diligence in infection prevention.
How Do AORN and CDC Guidelines Inform Cleaning Practices?
AORN and CDC guidance provide actionable recommendations for the frequency of cleaning, the sequence of cleaning tasks (top-to-bottom, clean-to-dirty), selection of disinfectants, and the use of PPE during environmental services. Both organisations emphasise that turnover cleaning should prioritise high-touch surfaces and that terminal cleaning must include air-handling considerations and all horizontal and vertical surfaces. Mapping these recommendations to SOPs helps facilities set acceptable dwell times, verify cleaning outcomes with objective tests, and incorporate PPE protocols to protect staff and patients. Local adaptation is expected and recommended where facility constraints or clinical workflows require modified sequences or supplemental measures.
Applying these guidance documents translates high-level recommendations into operational checklists and competency standards that frontline teams can reliably follow.
What Are the Relevant Australian Healthcare Cleaning Regulations?
In Australia, disinfectant selection and infection prevention practices must align with national and state health department advisories and product labelling, with attention to TGA considerations where applicable for product claims. Facilities should reference state-level public health or health service guidelines for specific requirements and ensure documentation practices meet audit and accreditation standards. Record-keeping expectations typically include retained cleaning logs, incident records, and QA data that demonstrate compliance during inspections. Procuring products with appropriate evidence and following manufacturer instructions for contact times and safe use is critical to meeting regulatory obligations.
Translating these regulatory requirements into operational SOPs ensures that cleaning activities are defensible, auditable, and aligned with Australian health governance frameworks.
How Is Staff Training and PPE Usage Critical in Surgical Suite Cleaning?
Staff training and correct PPE use form the frontline defence against contamination and occupational exposure during surgical suite cleaning, combining competency in infection control principles with procedural skills for cleaning, disinfectant handling, and equipment care. Training modules should include aseptic technique, spill management, instrument handling interfaces with central sterile services, and the correct use of disinfectants and application methods. PPE protocols must specify selection (gloves, gowns, eye protection, masks), donning and doffing sequences to avoid self-contamination, and disposal or laundering procedures consistent with clinical waste policies. Competency verification and regular refresher sessions maintain skill currency and ensure that cleaning staff perform reliably under perioperative time pressures.
The next subsections detail typical training topics and practical PPE protocols that support safe and effective sterile environment maintenance.
What Specialised Training Do Cleaners Receive for Infection Control?
Specialised training for cleaners in surgical environments typically includes modules on blood and body fluid management, aseptic cleaning principles, instrument pre-cleaning handover protocols, safe use and storage of disinfectants, and documentation requirements. Competency assessments may combine observed practical tasks, written checks on SOP knowledge, and periodic audits tied to QA results; refresher training is often scheduled annually or more frequently when metrics indicate gaps. Training records are maintained to demonstrate staff qualifications and to support retraining after incidents. Emphasis on understanding the rationale behind procedures improves adherence and enables cleaners to make safe decisions during unexpected events.
Embedding competency verification into the training program ensures that cleaning staff meet operational expectations and align with facility infection control goals.
How Is Proper PPE Use Ensured During Cleaning Procedures?
Ensuring proper PPE use involves clear SOPs that define which items are required for specific tasks, a standardised donning and doffing sequence to minimise contamination risk, and routine audits to check compliance and fit. Typical PPE for OR cleaning includes disposable gloves, fluid-resistant gowns or aprons, eye protection, and surgical masks or respirators where aerosol risk exists; escalation to higher-level protection occurs for gross contamination or known infectious cases. Practical steps—such as performing hand hygiene before donning gloves, avoiding touching the face, and using designated disposal pathways—reduce exposure and cross-contamination. Monitoring includes spot checks, competency observations, and corrective coaching when non-compliance is observed.
Clear protocols and active supervision reinforce PPE practices that protect staff and help preserve the sterile environment for patients.
What Are the Key Areas and Techniques for Effective Surgical Suite Sterilisation?
Effective sterilisation of a surgical suite focuses on risk-prioritised areas and uses compatible techniques matched to each surface or item: high-touch surfaces, surgical lights, operating tables, monitors, door handles, ventilation grills, and instruments all require specific approaches. The core technique is top-to-bottom cleaning combined with targeted disinfection of high-touch points, supplemented by appropriate instrument pre-cleaning before transfer to central sterile services. Adjunct technologies such as UV-C or hydrogen peroxide vapour can serve as supplementary measures when validated for the environment, but they do not replace manual cleaning where gross soil is present. Mapping areas to methods and agents provides frontline teams with practical guidance for consistent performance.
The table links common operating room areas and items to recommended cleaning techniques and approved agents for practical on-shift reference.
| Area / Item | Recommended Technique | Recommended Agent |
|---|---|---|
| Surgical lights | Wipe with microfibre cloth top-to-bottom; focus on handles and control panels | Hydrogen peroxide wipe or compatible QAC |
| Operating table and rails | Remove gross soil; wipe seams and controls; protect mattress per manufacturer | Alcohol wipe for controls; hydrogen peroxide for surfaces |
| Monitors and touchscreens | Use low-moisture wipe technique; avoid overspray | 70% isopropyl alcohol or manufacturer-approved disinfectant |
| Ventilation grills and high-level surfaces | Dust and vacuum as needed; wipe accessible grills and surrounds | Hydrogen peroxide solution or chlorine for outbreaks |
How Are High-Touch Surfaces and Surgical Instruments Disinfected?
High-touch surfaces are disinfected using a wipe-discard-wipe method with an appropriate agent and verified dwell time; sequence should move from least to most contaminated areas and from high to low elevation to prevent recontamination. For surgical instruments, front-line staff perform pre-cleaning to remove gross soil and then hand instruments over to central sterile services for validated reprocessing such as ultrasonic cleaning and autoclaving; cleaning staff must not perform terminal sterilisation of instruments themselves unless trained and authorised. Chain-of-custody and clear handover documentation reduce the risk of instrument contamination and ensure that reprocessing responsibilities are clearly assigned. Using appropriate PPE and avoiding direct contact with contaminated instrument lumens are essential to prevent exposure.
Maintaining defined boundaries between environmental cleaning duties and instrument reprocessing safeguards both patient safety and staff responsibilities.
What Role Does Environmental Hygiene Play in Preventing HAIs?
Environmental hygiene directly impacts HAI risk by reducing environmental reservoirs of pathogens and interrupting transmission pathways through systematic cleaning, disinfection, and monitoring. Recent studies indicate that improved environmental cleaning—coupled with hand hygiene and appropriate PPE—can reduce rates of certain HAIs, particularly those linked to surface contamination. Recommended KPIs include ATP results, frequency of thorough cleaning cycles, and microbiological swab trends, with routine review to detect patterns that warrant intervention. Continuous improvement loops that combine audit data, retraining, and targeted remediation sustain high performance and demonstrate to clinical governance how cleaning activities contribute to patient safety.
- Regular KPI monitoring reinforces accountability and identifies problem areas.
- Objective testing (ATP/microbial swabs) provides measurable evidence of cleaning effectiveness.
- Continuous training and process refinement ensure long-term reductions in HAI risk.
For support implementing tailored cleaning programs or requesting a quote, Divine Commercial Cleaning provides customised medical facility cleaning solutions across the Sunshine Coast and Brisbane. Their services focus on experienced professional cleaners, customised solutions, no lock-in contracts, environmental consciousness, police checks, and a money-back guarantee while aligning SOPs with clinical requirements and QA expectations.

Dianne, originally from Rockhampton, hails from a business-oriented family, with her father owning electrical stores and her uncle serving as Mayor. Moving to the Sunshine Coast at 13, she later pursued a rewarding real estate career and raised three children. As a single mom, she balanced university studies with domestic cleaning work. Armed with a Bachelor’s Degree in Business, majoring in Supply Chain Management, Dianne founded and grew Divine Commercial Cleaning into a thriving company. Her success is rooted in strong family mentorship, a positive attitude, and a solution-oriented approach, offering tailored cleaning services with integrity and strategic insight.

